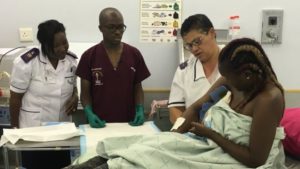
Dr Tjamena Murangi is among the first medical graduates to have been trained in Namibia.
Dr. Tjamena Murangi is seeing to a patient with a large infected wound on her arm — it is swollen and has lost color.
“Sorry Sisi, sorry,” he says in his soft-spoken voice as he gently cleans her wound.
His patient sits still but her face contorts with pain in a hospital ward in Namibia’s capital, Windhoek. The wards are busy on this Monday morning and scores are waiting to be treated in the emergency department.
The 25-year-old is slight but has a quiet confidence about him and people here in Katutura hospital seem to trust him. He was one of 37 in the first class of locally trained doctors to graduate earlier this year.
Until 2010, when the country’s first medical school opened, would-be doctors had to travel abroad — to South Africa, Russia, Cuba, Algeria and China — to be educated.
So Murangi is in the vanguard of something which could see a transformation in the health service here.
Namibia is a vast country but has a population of just 2.5 million, which is scattered in mostly rural and arid regions. This means that doctors are concentrated in urban areas and sometimes people have to travel a long way to get treated.
This morning some have traveled more than 50km (30 miles) to get to Katutura hospital. They wait quietly, but the doctors are feeling the pressure.
“Sometimes the workload can get quite overwhelming, you find that you have many patients to see and you get fatigued. You don’t have time to rest. This can really negatively affect patient care,” Murangi tells the BBC.
But things are improving and many here believe that the country’s new medical school presents a lasting solution to the problem of a lack of doctors.
The World Health Organization (WHO) has said that the shortage of medical staff in the public health sector here has hindered Namibia’s development.
One of the reasons behind the shortage is that it was only since independence from South Africa’s apartheid government in 1990 that health services were made available to the majority of people in Namibia, experts say.
A high HIV rate, shortage of medication in rural hospitals, limited training facilities, old infrastructure and a lack of equipment to treat patients have compounded the problem.
But Deputy Health Minister Juliet Kavetuna, who describes the sector as “fragile”, says she believes the country is now on the right track.
Read more here.


